Applications of genome editing technology in the targeted therapy of human diseases: mechanisms, advances and prospects
Pediatric Thalassemia And Your Child
Thalassemia is a common genetic condition affecting red blood cells. Children with severe forms of thalassemia often develop symptoms early in life, but effective treatment can manage the condition.
Thalassemia is an inherited (genetic) blood disorder that affects the production of hemoglobin, a protein that helps red blood cells carry oxygen.
Thalassemia is very common, affecting 18 per 100,000 people worldwide. It's considered pediatric when it affects children.
The symptoms of thalassemia can vary widely depending on the genetic mutations. It's also possible to have thalassemia along with other conditions that also affect hemoglobin, such as sickle cell trait.
In thalassemia, you inherit changes in the genes responsible for building hemoglobin, the main oxygen-carrying part of your red blood cells.
There are two main types of thalassemia: alpha-thalassemia and beta-thalassemia.
Most healthy hemoglobin includes two proteins: alpha-globin and two beta-globin. Inheriting faulty alpha-globin genes causes alpha-thalassemia. Likewise, inheriting faulty beta-globin genes results in beta-thalassemia.
The altered hemoglobin made by these faulty globin genes makes red blood cells small, fragile, and ineffective. These ineffective red blood cells cause microcytic anemia and other conditions.
Pediatric thalassemia symptoms are lifelong. In more severe forms of alpha- and beta-thalassemia, symptoms are usually present by 2 years old.
The most common issue of pediatric thalassemia is microcytic anemia, which is low hemoglobin with small red blood cells. Depending on the type of thalassemia you have, anemia can range from mild to severe.
Anemia can cause symptoms in children like:
As their bodies urgently try to produce more red blood cells, other organs other than the bone marrow may be affected. This can lead to symptoms like:
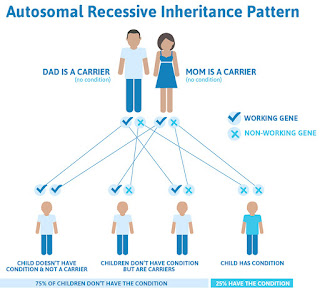
Thalassemia is inherited. In an autosomal-recessive pattern, children inherit the genes responsible for building healthy hemoglobin from their parents.
The genes involved in causing thalassemia include:
Alpha-globin genes
People have four alpha-globin genes located on chromosome 16. More than 130 possible changes to these genes are associated with alpha-thalassemia.
There are several types of alpha-thalassemia, including:
Alpha-thalassemia trait
If a child inherits one or two faulty alpha-globin genes, they have alpha-thalassemia trait, also called alpha-thalassemia minima/silent carrier or alpha-thalassemia minor.
This type may cause mild anemia with small red blood cells. But because their body can still make enough healthy hemoglobin, alpha-thalassemia trait usually won't cause any symptoms.
Alpha-thalassemia disease
Inheriting three faulty alpha-globin genes causes more significant problems. This is called alpha-thalassemia disease or hemoglobin H disease.
Depending on the type of gene mutations a child inherits, symptoms can range from mild to severe.
Hemoglobin Barts disease
Sometimes, a fetus may inherit problems with all four alpha globin genes. This extremely severe form of alpha-thalassemia disease is called hemoglobin Barts disease. It causes severe hydrops fetalis and is often fatal before birth.
Beta-globin gene
This gene is located on chromosome 11. More than 200 mutations in it are associated with beta-thalassemia.
There are several types of beta-thalassemia, including:
Beta-thalassemia trait
If a child inherits problems with one of two beta-globin genes, they'll have the beta-thalassemia trait. This causes mild anemia with small red blood cells. But they still have one functional beta-globin gene and plenty of healthy hemoglobin, so their anemia is typically asymptomatic.
Beta-thalassemia disease
In this case, both of the beta-globin genes are mutated. Depending on the type of mutation a child inherits, they might develop beta-thalassemia intermedia with fewer symptoms when at least one of their beta-globin genes can still make a reduced amount of normal beta-globin.
They may also develop beta-thalassemia major or Cooley anemia if their body is unable to make any healthy beta-globin. Symptoms of Cooley anemia start early in life and are very serious, requiring repeated blood transfusions.
Children with thalassemia trait or thalassemia minor are unlikely to develop significant symptoms or require treatment. The thalassemia trait does not develop into thalassemia disease.
Children with thalassemia disease need lifelong care from a hematologist. Treatment can help manage their anemia, ineffective red blood cell production, and any complications.
The outlook for children with thalassemia has significantly improved over recent decades. Advances in the monitoring and treatment of iron overload, along with newer gene therapies, can manage symptoms and lengthen the life span of people with transfusion-dependent thalassemia disease.
Thalassemias are a common group of inherited blood disorders. People are born with the condition.
Thalassemia trait, also called thalassemia minor, rarely causes significant health problems. But children with alpha- or beta-thalassemia disease may experience anemia and problems with the bones and organs.
Symptoms of pediatric thalassemia usually develop in infancy or young childhood. In the most severe forms, frequent blood transfusions may be necessary.
If your child has thalassemia, an experienced pediatric hematologist can help. Therapy is available to monitor for, prevent, and treat some of the most serious complications of thalassemia disease.
How Reblozyl Works For Anemia
Your blood carries oxygen to all of the cells in your body. When there are problems with red blood cells, you can feel weak and tired and may have to take medicines or receive blood transfusions to manage this.
Reblozyl (REB-low-zil) was approved in 2019 and is the first erythroid maturation agent (EMA) that helps to mature red blood cells in people with anemia (low red blood cells) caused by certain blood disorders.
Reblozyl is used to treat anemia in adults with the following:
Beta-thalassemia is a condition where your body does not make enough hemoglobin, a protein that your blood cells use to carry oxygen. This can make it more difficult for oxygen to get delivered to your body.
Myelodysplastic syndromes (MDS) are a type of cancer where your bone marrow does not make enough healthy blood cells. It can happen if there is a mutation in your DNA, which can change the way your cells grow and function. The bone marrow makes blood cells for your body including red blood cells, which carry oxygen, white blood cells, which fight infections, and platelets, which help your blood to clot. An erythropoiesis-stimulating agent (ESA) is a medicine that tells your body to make more red blood cells.
Beta-thalassemia and MDS can cause anemia. Reblozyl is approved to treat anemia if you have either of these conditions. Reblozyl increases the number of red blood cells by allowing immature red blood cells to mature. This allows the quality of red blood cells to improve and increases the amount of hemoglobin in the blood, allowing your blood to carry more oxygen. Because of this, Reblozyl may help lower the amount of blood transfusions you may need. Reblozyl is not a substitute for blood transfusions.
Reblozyl is given by a health care provider as an injection once every 3 weeks in your upper arm, thigh, or stomach. It is given at your health care provider's office. If you miss your dose of Reblozyl, call your health care provider right away. Try to keep all appointments with your health care provider to receive Reblozyl. It may be helpful to write down your symptoms in a notebook or on your phone so that you and your health care provider can discuss how Reblozyl is working for you. The amount of Reblozyl you receive will depend on how much you weigh and how you respond to the medicine.
One study was conducted in people with beta-thalassemia that required regular blood transfusions. People received either Reblozyl or a placebo containing no medicine. The study looked to see the percentage of people who had a reduction in the number of blood transfusions they needed (by 33% or more) plus a reduction in the amount of blood needed for the transfusion from week 13 through week 24. The median age in the study was 30 years old and included White people (54.2%), Asian people (34.8%), Black people (0.3%), and those classified as "Other," (7.7%) including those classified as Hispanic or Latino (2.1%).
Two studies were conducted on people with MDS. The first study looked at people with anemia due to MDS who had never received an erythropoiesis-stimulating agent (ESA) and were receiving blood transfusions. People received either Reblozyl or epoetin alfa, which is an ESA. The study looked to see the percentage of people who did not need blood transfusions for at least 12 weeks and had an increase in hemoglobin by 1.5 g/dL. The median age in the study was 74 and included White people (79%), Asian people (12%), Black people (1%), and those classified as "Unknown," (8%) including those classified as Hispanic or Latino (6%).
The second study looked at people with anemia and MDS where an ESA medicine was not effective and were receiving regular blood transfusions. People received either Reblozyl or a placebo. The study looked at the percentage of people who did not need blood transfusions for 8 weeks or longer. The median age in the study was 71 and included White people (69%), Black people (0.4%), and those classified as "Other," (0.9%) including those classified as Hispanic or Latino (3.1%).
Beta-thalassemia. People in the Reblozyl group had a greater percentage of people (21.4%) who needed fewer blood transfusions and a lower amount of blood needed during those transfusions compared to placebo (4.5%).
Myelodysplastic syndromes. In people who had never received an ESA, Reblozyl had a greater percentage of people (59%) who did not need a blood transfusion and had an increase in hemoglobin compared to epoetin alfa (31%).
In people who had received ESA in the past and had used an ESA medicine that was not effective, more people in the Reblozyl group (38%) did not need a blood transfusion for 8 weeks compared to placebo (13%).
These three clinical studies showed that Reblozyl lowered the severity of anemia and the number of blood transfusions needed in people with beta-thalassemia or MDS.
Reblozyl may take a few weeks to work to lower your need to have blood transfusions due to your anemia. Your health care provider will monitor you while you are receiving Reblozyl. Your health care provider may adjust your dose or stop treatment with Reblozyl depending on how you respond to the medicine.
The most common side effects seen with Reblozyl are:
Receiving Reblozyl can cause tiredness, dizziness, or cause you to feel off-balance. It is important not to drive or operate heavy machinery until you know how Reblozyl affects you.
Headaches as well as muscle or joint pain can happen while taking Reblozyl. Taking over-the-counter medicines such as Tylenol or ibuprofen can help. Call your health care provider if these symptoms do not go away or get worse.
Reblozyl can cause nausea, diarrhea, and stomach pain. Eating smaller, more frequent meals may help alongside eating bland foods such as bread, plain crackers, and rice. It is also important to stay hydrated and to drink plenty of water. Your health care provider may tell you to keep certain over-the-counter medicines on hand in case of these side effects. Call your health care provider if your symptoms do not improve or get worse.
You can develop a cough from receiving Reblozyl. Call your health care provider if this becomes bothersome.
Receiving Reblozyl can cause an allergic reaction and shortness of breath. Talk to your health care provider about the symptoms of an allergic reaction. Your health care provider may monitor you immediately after receiving Reblozyl. Call your health care provider right away or go to the nearest emergency room if you have symptoms of an allergic reaction.
Reblozyl can increase your risk of developing COVID-19. These symptoms may include fever, cough, chills, and body aches. If you test positive for COVID-19, call your health care provider. Make sure you isolate yourself from others and wear a mask when out in public to prevent spreading the infections to others.
Reblozyl can cause your body to hold fluid, which can lead to swelling. Call your health care provider if you experience this. Your health care provider may give you medicine to help with this.
Reblozyl can also cause high blood pressure. There are techniques that you can implement to help control your blood pressure. This includes exercising regularly and following the DASH diet, which includes fruits, vegetables, and low-fat or nonfat dairy products. It also limits alcohol, smoking, trans and saturated fats, and sodium. Call your health care provider if you notice your blood pressure increasing and go to the emergency room if the top number (systolic) of your blood pressure is over 180 or if the bottom number (diastolic) of your blood pressure is over 120.
Taking hormone replacement therapy, which can be used for menopause, or birth control with Reblozyl can increase your risk of developing blood clots. Tell your health care provider about all the medicines you are taking including prescription and over-the-counter medicines, vitamins, and herbal supplements.
The manufacturer has a program that can provide information about financial support options for Reblozyl. If you have beta-thalassemia, you can find out more at www.Reblozyl.Com/beta-thalassemia/resources/financial-assistance. If you have MDS, you can find out more at www.Reblozyl.Com/mds/resources/financial-assistance. You can also call 800-861-0048.
What Are The Different Types Of Anemia?
Although all types of anemia are characterized by dysfunctional or low levels of red blood cells, the causes, severity, and treatment of the different kinds of anemia can vary.
Anemia is a health condition that occurs when you don't have enough red blood cells or when the red blood cells in your body are unable to function properly. Anemia can cause symptoms like fatigue, dizziness, and shortness of breath.
There are many types of anemia, including:
Some can be treated easily and resolved quickly. Other types require more intensive, possibly lifelong treatment.
This article looks at the different types of anemia, their causes, and treatment options.
Although all anemia types are characterized by low red blood cell levels or red blood cells that don't work as they should, there can be significant differences in each type's causes, severity, and treatment.
Anemia is typically diagnosed with blood tests that examine the number, shape, and health of red blood cells. If you receive a diagnosis of anemia, treatment depends on the type.
Anemia typically has three main types, each of which can have different causes:
Symptoms
The symptoms of all types of anemia can be similar and may include:
Let's take a closer look at these three types of anemia in more detail.
In microcytic anemia, red blood cells are smaller than they should be. This happens because your red blood cells don't have enough hemoglobin, a protein in red blood cells that helps carry oxygen through your bloodstream and throughout your body.
Causes
Types of conditions that can cause microcytic anemia include:
Treatment
The treatment of microcytic anemia depends on the underlying cause. For instance:
With normocytic anemia, red blood cells are all the same size, but there aren't sufficient circulating red blood cells to meet the body's needs.
Normocytic anemia most often results from an underlying chronic illness. Less frequently, you may be born with it, or it can be a side effect of a medication.
Causes
The most common conditions that can affect red blood cell production and lead to normocytic anemia include:
Treatment
The treatment of normocytic anemia depends on the underlying cause.
With macrocytic anemia, the bone marrow makes red blood cells that are larger in size than typical red blood cells. This type of anemia can develop if the body lacks certain nutrients.
There are two kinds of macrocytic anemia: megaloblastic anemia and nonmegaloblastic anemia.
Megaloblastic anemia
Megaloblastic anemia happens when you don't get enough vitamin B12 or folate. If your body doesn't have enough of these nutrients, the bone marrow has a hard time making healthy red blood cells.
Treatment of megaloblastic anemia may include taking vitamin B12 and folate supplements and increasing your dietary intake of these vitamins.
Some people have an autoimmune condition called "pernicious anemia" that prevents their bodies from absorbing vitamin B12. If untreated, pernicious anemia can cause irreversible damage to the nervous and digestive systems.
Treating pernicious anemia usually involves vitamin B12 injections, which are given daily or weekly until B12 levels are within a healthy range.
Nonmegaloblastic anemia
With nonmegaloblastic anemia, certain medical conditions may affect how easily the body absorbs nutrients needed for healthy red blood cell production. The most common conditions that can cause nonmegaloblastic anemia include:
If you have nonmegaloblastic anemia from an underlying chronic condition, doctors usually focus on treating the underlying disease.
Anemia is a health condition that occurs when you don't have enough red blood cells or your red blood cells can't function properly. It can cause symptoms such as:
The different types of anemia share similar symptoms but have different causes, treatments, and severity. Some anemias, such as megaloblastic anemia, can be treated with dietary changes. Other anemias, such as sickle cell anemia, are chronic and inherited.
You can't prevent inherited types of anemia, but you can take steps to help your body get the nutrients it needs to prevent anemias caused by a lack of iron, B12, or folate.

Comments
Post a Comment